
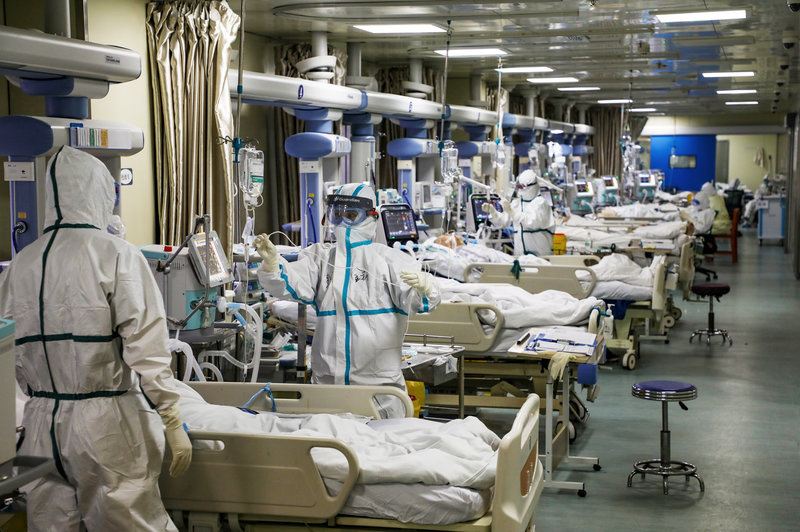
Featured image: A medic looks at a patient who has shown symptoms of COVID-19 at an isolation ward in Hyderabad. Photo: PTI
“Few things (are) guaranteed in life. Death is the most certain of them. But what we die of has and is continuing to change.”
COVID-19 and the devastation it has caused across the globe was nowhere on the horizon of healthcare concerns when BBC health correspondent Nick Triggle wrote thus in his perceptive article. Ironically, the article, published in April 2015, even had a suggestion that advances in medical sciences – particularly vaccines – have reduced the burden of infectious illnesses significantly. Still, looking back at the article as the COVID-19 pandemic ravages country after country, Triggle’s point that “what we die of has and is continuing to change”, is marked by extraordinary intuition. But it is not just the way humankind dies that is changing in the times of this pandemic. The way we perceive death and undergo grief has also changed strikingly. Even the manner in which health workers relate and respond to deaths has altered dramatically.
The increasing numbers of COVID-19 patients and those dying across India instil fear among not only those who are informed that they have symptoms of the disease, but also among the vulnerable – the elderly and the ones with comorbidities.
The process of dying is becoming one of extreme anguish not only for those dying from COVID-19, but their families and the ones who watch over them in the hospitals. The anticipation of death is also viewed with dread among non-COVID-19 patients (those with incurable advanced illnesses like cancer, end-stage organ failure and other emergencies). Healthcare workers taking care of non-COVID-19 patients are also going through a very tough period where they, instead of saying, “We will do everything we can, and be there with you through this journey,” are saying, “We will be able to do only this much, hope you understand.” For a person who is working in palliative care, offering comprehensive care in serious health-related suffering and maintaining dignity during the process of dying, this could add an overwhelming sense of helplessness and guilt.
A fellow doctor who witnessed a COVID-19 patient die says that the trauma of watching the ‘air hunger’ of the deceased during his last moments has left a permanent scar on his mind. A colleague in palliative care lost her brother in intensive care in Bangalore a few days ago. While she could get a glimpse of him before he died through a WhatsApp video, her mother couldn’t see him at all. The way he died and the quick cremation that had to be carried out has pushed the entire family into inconsolable, extremely painful grief.
As a palliative care physician, my colleague reaches out to patients who are dying day and night, but she is still not able to come to terms with the atmosphere of “intense isolation” that preceded her brother’s death. Some of the decisions that we are constrained to take in relation to patients not inflicted by COVID-19 is also extremely disconcerting in the present context. An advanced breast cancer patient had come to the hospital, clearly in her last stages. When this prognosis became known, her husband kept requesting that the patient be taken home, but we were not confident enough to respect the request on account of the pandemic. There was no other way but to negotiate with death in the hospital.
The mental agony of a pandemic
As is well known, COVID-19 mortality rates are the highest among the elderly: 3-11% in those aged 65-84 and 10-27% in those over the age of 85. Among these, those who have multiple comorbidities, and individuals on multiple medications experience higher rates of morbidity and mortality. Apart from the trauma caused by illness and death, other losses ranging from that of livelihood, financial security, personal freedom and control over one’s own life have compounded mental health issues of people across the globe. The abject disruption of sectors like education, employment, transport, agriculture, industry and healthcare has also aggravated the sense of collective loss and grief in the community.
Also Read: When a Pandemic Begins, a Mental Health Crisis Threatens to Follow
Indeed, along with the new conditions of deaths that the pandemic has inflicted on the world, the mental stress and agony that has come along with it also have new and excruciating nuances. And like the pandemic, these psychological and psychosocial traumas are also globally felt. Studies from countries like China and Italy have reported significant distress. The survey in China during the initial outbreak shows that psychological impact on 53.8% of the respondents was moderate to severe. In Italy, COVID-19 related anxiety was reported as high as 73.9% of those took the survey. These studies went on to record that the situation could have serious negative effects on the mental health of the population as a whole.
Evidently, these studies highlight that the risk of psychological morbidity is higher among the elderly, vulnerable and women. For example, a study in the UK, the Black, Asian and Minority Ethnic (BAME) patients have a higher proportion of deaths in intensive care compared to White Caucasians, and 72% of males being affected compared to 28% in females.
Reports from other parts of the globe also underline that collective anxiety has become a worldwide phenomenon with the increasing infection rates and deaths due to COVID-19. In India too, fears of contracting the disease along with constant apprehensions about health and safety have recorded a phenomenal rise. Central to these fears and apprehensions are the loss of connectedness, uncertainty about the future and the loss of control over day-to-day life. Consequently, it has practically overwhelmed the normal skills of adaptability and problem-solving in a large number of individuals. The dramatic feeds and visuals propagated by a large section of the media also contribute to precipitating panic and a sense of impending doom. Combined with all this, the prolonged physical distancing and the resultant social isolation have also been found to impact the collective psyche adversely.

A multi-pronged approach is must
So, how do health workers, specifically medical practitioners who are specialised in palliative care and psychosocial care, contribute to this unique situation? To start with, communicating in challenging situations, discussion regarding goals of care with the patients and families is a must, as those with severe conditions may deteriorate rapidly and go through a totally unpredictable disease trajectory. Parallelly, they should empower health workers in the skills that are very needed currently.
The rapid deterioration in COVID-19 leaves the family unprepared to cope with the loss. The process of grief that follows is by and large accompanied by guilt, blame, anger and hostile reactions. There are times that this could be especially targeted at healthcare professionals and public systems.
The stringent controls on public movement and social interaction are bound to prevent conventional mourning practices and social goodbyes, leading to further precipitation of such extreme reactions. For large sections of Indian society, rites and rituals after bereavement are an essential aspect of mourning and imperative for the liberation of the soul. Families unable to be by the patient’s side at the time of death or during last rites may experience lingering mental health issues.
Thus the collective, community-oriented sense of loss in a pandemic is experienced not only at the individual and family level, but also at the socioeconomic and political level. Facilitating meaningful final goodbyes and funerals, conducted virtually over the phone or social media platforms, may aid grieving and limit the hostile reaction. Addressing the distress and establishing care pathways along with the general measures is possible. This has been recommended by palliative care globally.
Stigmatisation increases anxiety
Another long-standing factor that aggravates collective anxiety in the Indian context is the social stigma associated with the illness. Not only those who have taken in ill and their families are targeted, but there is also a steady stream of reports about attacks on healthcare workers. So much so, even the after death, healthcare workers were being discriminated against, denying them a decent burial. Needless to say, this denial of dignity in care at the end-of-life is bound to add to the emotional distress of the family. It is important to address the social stigma associated with COVID-19 through clear information and guidelines.
Frontline medical workers who are engaged directly in screening, triaging and treatment of COVID-19 patients are at increased risk of psychological morbidities like anxiety, stress, depression, burnout and post-traumatic stress disorder as a result of responding to the pandemic. There is widespread fear about India’s public healthcare system’s inability to handle the surge of critically ill patients.
Also Read: Next Barrier After COVID-19: Stigma and Discrimination in the Time of Pandemic
Clinicians forced to care for an increased number of patients, in a new and unfamiliar work environment, for long hours, in the discomfort of wearing personal protective equipment (PPE), report physical and emotional exhaustion. Work stress is compounded by the personal fear of contracting the illness and infecting one’s families, the physical distancing from the families, and the stigma and avoidance by society.

As noted by Downar J., and Seccareccia D., in their study, published in the Journal of Pain and Symptom Management in February 2010, this distress is further amplified on account of factors like shortage of staff, supplies and space, and the absence of clear-cut decision-making guidelines and organizational support for frontline workers.
The viewpoints of those affected by the pandemic and those who are trying to give care in these difficult circumstances clearly indicate that integrating palliative care and psychosocial interventions into the scheme for general disease prevention and treatment is absolutely imperative.
Also Read: How the Social and Behavioural Sciences Can Help Us Beat the Pandemic
Time and again, it has been proven that this type of comprehensive planning and implementation have helped to lessen the risk of mental health morbidity and enable social stability, the latter being an integral factor in combating the new and inexplicable times created by the pandemic.
Dr Chitra Venkateswaran, associate professor and head, Department of Psychiatry and Palliative Care, BC MCH, Tiruvalla, Kerala, India. She is also clinical director, Mehac Foundation, Kochi, Kerala. She can be contacted at chitven@gmail.com.
Dr Seema Rajesh Rao, MBBS, DPM, MSc (Pall Med), consultant, Department of Palliative Medicine and Supportive Care, Kasturba Medical College and Hospital, Manipal. She is honorary tutor, School of Medicine, Cardiff (UK). She can be contacted at uskpsy69@gmail.com.
Denny John is an economic epidemiologist and is adjunct faculty at Amrita Institute of Medical Sciences (AIMS), Kochi. He tweets at @djohn1976.

